In a new blog series, we will be reimagining policy.
City-REDI will be giving talented young voices in the West Midlands a chance to shine.
First in the series is Nikita Samoylenko, a MSc. Economics Graduate from the University of Warwick.
The Independent Investigation of the National Health Service in England, widely known as the Lord Darzi Report, offered a stark assessment of the key challenges facing the National Health Service and the broader health of the UK population in the aftermath of the Covid-19 pandemic.
The report finds that the demand for healthcare has risen with more reported cases of chronic illnesses and mental health conditions such as depression, stress, and anxiety persisting well above their pre-pandemic levels. A stretched NHS has struggled to keep up with the growing surge of cases and to provide accessible care to a population in dire need of stronger health services in the post-Covid landscape.
The Covid-19 Pandemic Reshaped the UK Labour Market
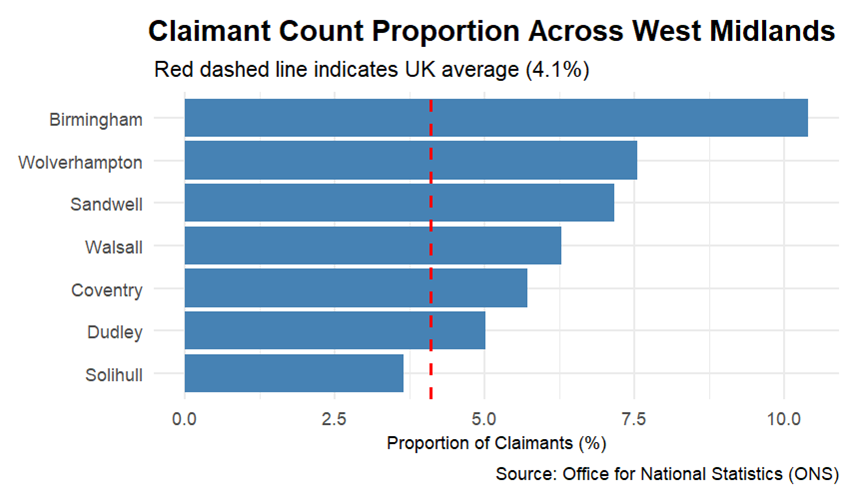
Yet, the consequences of the pandemic are not confined to health alone. The pandemic dramatically reshaped the labour market as hundreds of thousands of workers withdrew from the labour force due to the scale of increase in work limiting-health problems, poor population health, and an increase of retirees. Across the Midlands, the gaps in both unemployment and health have widened, revealing not only a rise in regional inequality, but also a stark contrast within West Midlands communities. Particularly, Job Seeker’s allowance and Out of Work Universal Credit claims across the West Midlands communities range significantly and point to growing interregional labour disparities. For example, Birmingham exceeds the national average by more than twofold, while some areas, like Solihull, fall below the average UK claimant rate (see Figure 1).
Figure 1: Job Seeker’s and Universal Claimant Count Proportion July 2024 to June 2025
Regional inequality within the UK, and particularly the Midlands region, is pronounced and mirrors broader deprivation of social determinants of health (SDOH) such as income, healthcare access, and education, among other factors. Areas with higher unemployment and lower average incomes tend to have a higher percentage of adults with no formal educational qualifications. Persistent high unemployment can discourage skills and educational attainment, especially among the younger population. Youth unemployment has consequently suffered, as there are currently 29,000 unemployed young people in the West Midlands as of November 2025, with rates double the national average in areas such as Birmingham, Walsall, and Wolverhampton.
To help the youth NEET (Not in Employment, Education, or Training) population, West Midlands Mayor Richard Parker has launched a new innovative scheme, , in cojunction with the West Midlands Local Authorities. The initiative aims to connect young minds with businesses and support their transition into employment. Lower youth unemployment and greater direct skills accumulation are beneficial for the region and are imperative for long-term growth, productivity, and innovation. Active labour market initiatives, such as YouthPath, can help discover the untapped pool of talent in the region. Implementing job schemes to get individuals back to economic participation will play a major role in boosting regional economic prosperity. However, unemployment is only a single aspect of the problem. An equally formidable challenge of narrowing health inequalities across regions through early detection and prevention policies lies ahead.
Health Deprivation in the West Midlands
The Index of Multiple Deprivation (IMD), published in 2025, is the UK’s official measure of relative deprivation across local authorities within the United Kingdom. Birmingham scores particularly low on the health and disability metric, which measures the risk of premature death and reduced quality of life due to poor physical and mental health and accounts for 13.5% of the total deprivation score. The IMD reports Birmingham to be more deprived than 92% of all local authority districts in England on the health and disability category, which reflects the growing burden of chronic illness, mental health challenges, and lack of readily accessible, high-quality healthcare intertwining with lower employment outcomes. A recent article by Leszek Rzesniowiecki finds that 40% of people living in workless households in the West Midlands are out of work due to long-term sickness. These findings reveal a deepening regional health crisis with mounting implications for the future of the labour force. Higher rates of chronic illnesses withhold many from employment, and for those in employment, workplace factors have contributed to poor health outcomes. Figure 2 plots workdays lost by UK region.
Figure 2: Average Number of Workdays Lost Across the 3-year period 2022/2023-2024/25.
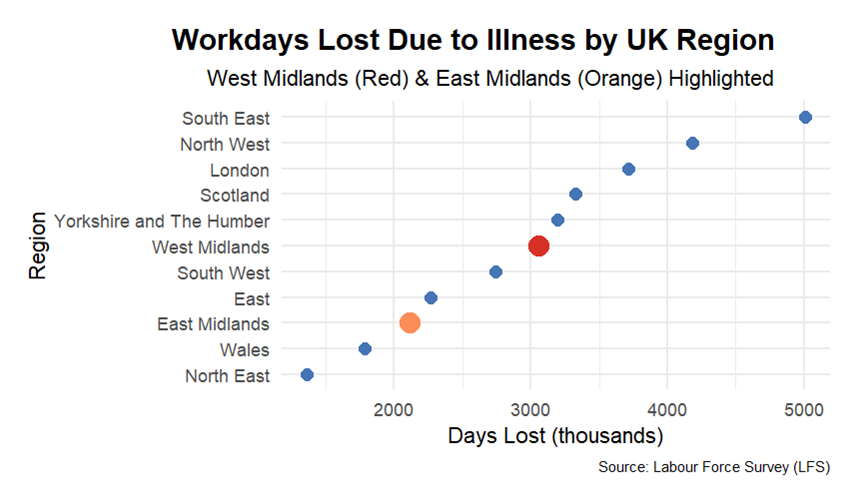
The interregional range of workdays lost due to illness between the West and East Midlands reveals a divergence in health disparities. The East Midlands region reports some of the fewest workdays lost due to illness, while the West Midlands reports a figure closer to the national average. Higher rates of chronic illness, greater socioeconomic deprivation, and industries with more physically demanding labour and lower wage service jobs concentrated in the West Midlands are likely to contribute to the disparity compared to the East Midlands.
The Labour Force Survey reports that, due to musculoskeletal disorders caused or made worse by work, the West Midlands lost an estimated 703,000 workdays across the 3-year period of 2022/23-2024/25, while the East Midlands lost an estimated 220,000 workdays. The disproportionate loss of workdays experienced by the West Midlands will contribute to the disparity when compared with the neighbouring East Midlands. Higher workdays lost due to illness will hurt businesses through the loss of workers and lower output. Meanwhile, workers experiencing higher rates of illness can fall out of employment and see their ability to accumulate skills or education constrained.
However, the East and West Midlands perform similarly in terms of self-reported stress, depression, or anxiety caused or made worse by work, with the average days lost per worker being 0.61 and 0.66, respectively, compared to the overall estimated average days lost per worker in Great Britain (0.69). To understand the contrast within the Midlands region, it is essential to consider the broader challenges facing the NHS system across UK regions. Particularly, the NHS has struggled to scale down its waiting times and provide patients with further access to specialists.
A Stretched NHS is Struggling with Rising Healthcare Demand
Figure 3: Referral to Treatment (RTT) Waiting Times, Published May 2025 (Revised July 2025)
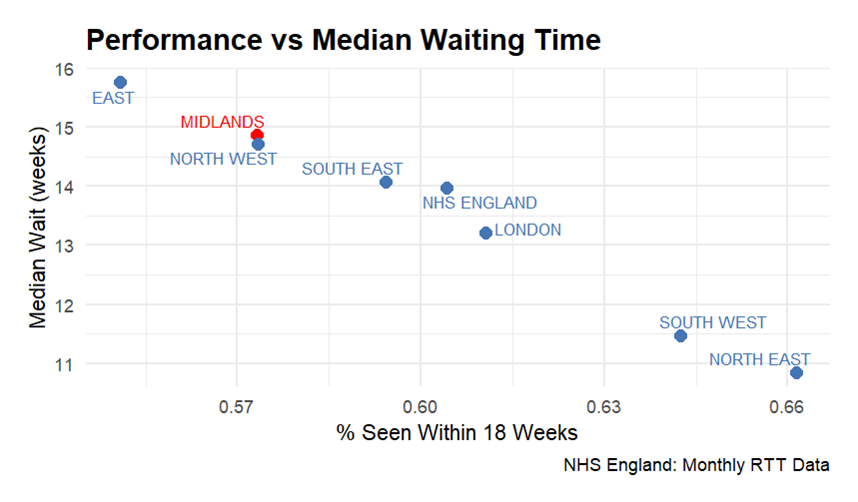
The NHS has set forth its national guidelines that the maximum wait time for non-urgent, consultant-led treatment is 18 weeks, thus setting the standard for all regional hospitals to follow. However, demand for healthcare has outpaced the ability of the NHS to provide timely services. The Midlands have some of the longest patient waiting times, and the percentage of patients seen by a practitioner within the NHS benchmark of 18 weeks is one of the lowest in the country, with only 57% of patients being seen by a practitioner in the allotted time frame. NHS show NHS Midland hospitals perform at similarly low levels, with no significant variation between the West or East Midland hospitals. With the West Midlands reporting a higher rate of self-reported sickness and chronic illness, NHS performance lies at the heart of addressing the issue of a sicker labour force and the consequent economic burden faced by the region.
Rising Healthcare Backlogs and Illness Prevalence
These systemic challenges faced by the National Health Service are becoming increasingly visible. In early December 2025, the King’s Mill Hospital in Sutton-in-Ashfield reported an influx of 220 patients, with 43 patients having to wait longer than 12 hours to be seen by a practitioner. The Lord Darzi Report finds that patients waiting for more than a week for a GP appointment rose to 33% in 2024 compared to 16% in 2021. In addition to longer waiting times, the Lord Darzi report finds that half of the 7.6 million patients waiting for elective treatment in 2024 were working-age adults.
Delayed treatment can negatively impact the health of working-age adults, causing many to drift in and out of employment. Unstable employment diminishes worker productivity and dissuades workers from upskilling. As workers are caught in a limbo where they are waiting long weeks to be seen by a practitioner, businesses are hurt as they are forced to have their employees work overtime or find temporary workers. Meanwhile, the long-term health of workers is jeopardized, which impacts lifetime earnings, education levels, and future long-term employment opportunities.
NHS: A Constant State of Crisis?
Frustration with the National Health Service has increasingly grown since the Covid-19 pandemic and has been reflected in the media. Greener and Powell (2024) find that the top NHS crises addressed by the media were the NHS’s poor performance in winter months and its issues with staff recruitment and retention. Both issues have escalated over recent years and have tainted the image of the NHS with the public.
However, the struggles of the NHS directly impact the Midlands economy. Particularly, the West Midlands experiences significantly more days lost due to illness than the East Midlands (Figure 2). As contagious diseases spread at higher rates during the winter, the seasonality of infectious illness rates can stunt the West Midlands economy at the beginning of each year. A sicker workforce entering the new year each year can also impact labour disparities between the East and West Midlands and pull more workers out of the labour force in the West Midlands compared to the East Midlands. It is imperative that NHS policy is tuned to serving the unique challenges of the region as less access to adequate healthcare will only increase the trend in sickness absences and reduce the region’s effective labour force.
Concluding Remarks
The health of the labour force is essential to ensuring a brighter future for the Midlands. Policy must take into consideration the dual nature of this issue. Matching businesses with young talent will help boost economic activity and address skill shortages, but it is equally important to ensure the health of the population through preventative and early detection policies. A coordinated effort is needed between local authorities, NHS hospitals, and employers to ensure skills development and health promotion are invested in and developed to appropriately address the challenges faced by the Midlands region.
This blog is written by Nikita Samoylenko, the University of Warwick.
Disclaimer:
The views expressed in this analysis post are those of the authors and not necessarily those of City-REDI or the University of Birmingham.
